Epidemiologists and virologists around the world are scrambling to understand and prevent the spread of the novel coronavirus. There is another group of researchers who are concerned about a slightly different foe: the mental health pandemic.

Facing an infectious disease, we have been forced to maintain distance from each other, all while going through levels of fear, uncertainty, job loss, and grief that are unprecedented for many people.
“In an ironic twist, many of the strategies that are critical to ensuring our collective public health during this pandemic may put people at greater risk for . . . mental health issues,” write Frederick Buttell and Regardt J. Ferreira at Tulane University in a recent, special issue of the journal Psychological Trauma.
In brand-new studies coming out of China, Spain, the United States, and other countries, researchers are discovering in real time how we are collectively coping with this worldwide event. The results are not uplifting, but they aren’t surprising either. We are suffering, some of us worse than others. You don’t have to have lost a job or a loved one to be affected. Humans are complex, and so are emotional responses to the pandemic.
When this all started, we learned how viruses spread and how to wash our hands like pros. Now we have lessons to learn about what happens to mental health in a crisis like this, so we can find ways to address it.
1. We’re anxious, depressed, and traumatized
As COVID-19 spread through China in January and February, researchers were already sending out questionnaires to citizens locked down in their homes. In half a dozen studies with over 10,000 respondents, they found that people were experiencing worse mental health problems than before the pandemic—high symptoms of stress, anxiety, depression, and post-traumatic stress disorder (PTSD). Up to half showed serious signs of depression (depending on the study), while up to 35 percent showed serious anxiety.
One survey followed over 1,700 people in 190 Chinese cities from late January to late February. During the height of the pandemic, their stress, anxiety, and depression didn’t change. Their symptoms of PTSD declined slightly—but they were still high enough to be worrisome. People weren’t getting worse, but they also didn’t seem to be getting used to pandemic life.
The results look no better in other countries. In late March, nearly 3,500 people were surveyed in Spain, when the country ranked second in the world in COVID-19 deaths. Many people met the criteria for clinical mental health problems: 19 percent for depression, almost a quarter for anxiety, and 16 percent for PTSD. Within a week after Slovenia declared an epidemic, over half of the thousands of people surveyed had high stress levels. In April, 14 percent of Americans were experiencing serious psychological distress, more than triple the rate in 2018.
And studies find that this stress and anxiety fuels poor sleep, creating a vicious cycle. The more we lay awake at night during the pandemic, rehashing worries we have no control over, the worse our mental health becomes.
2. Some of us are lonely, but not all
Stay-at-home orders and social distancing have left many people isolated, so it makes sense that we would be feeling lonely. And, indeed, nearly 1 in 7 U.S. adults said they were often or always lonely in April 2020, up over 25 percent from 2018. But another study in the U.S., Canada, and the U.K. found that people’s feelings of connection to others didn’t change much from before to during the pandemic. When one group of researchers surveyed over 1,500 people in the U.S. from January to April, they were surprised to find “remarkable resilience.” Not only did people not become lonelier over time, but they actually gained a greater sense of support from others.
All the phone calls and video chats with family and friends may be helping, write Martina Luchetti and her coauthors from Florida State University, as well as a new sense of togetherness. “Many people have felt part of community-wide efforts to slow the spread of the virus. The feeling of . . . being in this together may increase resilience.”
However, this hasn’t been true for everyone. People who are younger or living alone, or who have a chronic health condition, are lonelier than other groups. In fact, one study in the U.S. in April and May (before any restrictions were lifted) found that almost two thirds of people under 30 had high levels of loneliness, and 37 percent felt they had low support from their family.
“Feeling cut off from social groups may lead one to feel vulnerable and pessimistic about one’s circumstances,” write Cindy H. Liu and her coauthors.
3. Domestic violence has increased
In early April, the United Nations called for immediate global action to combat the increasing violence against women and girls during the pandemic.
According to news reports, domestic violence is increasing worldwide. At one police station just over 100 miles from Wuhan, China, for example, reports were three times higher in February 2020 compared to February 2019. In New Orleans, domestic aggravated assaults jumped 37 percent from January to April. Similar trends have been reported in Spain, Italy, Germany, and Brazil. As people are stuck at home, calls to helplines are surging.
Scientific surveys are only just beginning, but some preliminary results confirm these trends. Among people who were already experiencing domestic violence, the violence has gotten worse in nearly 60 percent of cases, report Buttell and Ferreira.
In their view, this comes down to a variety of factors: people spending more time at home with abusive partners, unemployment and other financial stressors causing conflict, shelters shutting their doors, and police being discouraged from making arrests.
Needless to say, the threat of abuse is compounding the stress, anxiety, and fear that many people are already experiencing during the pandemic.
4. The effects depend on your personality, lifestyle, and demographics
While older people have greater health risks from COVID-19, it seems to be younger people who are struggling emotionally. According to studies from Spain, China, and Slovenia, younger people tend to be more depressed, anxious, stressed, and traumatized in the era of COVID-19. The same is true for women, who may also be more lonely.
There’s no clear explanation for why this might be true, but researchers have some speculations. Women tend to have worse mental health in general, and certain stressors right now—like the added burden of caregiving and the risk of losing jobs—may fall more heavily on women.
For younger people, it could be the disruptions to their routines that are to blame, particularly for college students who have had to adjust to online schooling. In studies across both China and the United States, the more the pandemic was affecting people’s daily lives, the more anxious they felt.
Personality also influences how we fare in tough times. Two related traits that seem to matter during the pandemic are our ability to tolerate uncertainty and our ability to tolerate distress. While it’s hard for anyone to struggle or face the unknown, some people are less comfortable with it than others. And right now, it’s those people who seem to be ruminating more, feeling more afraid, and experiencing more depression, anxiety, and PTSD.
5. It’s worse for disadvantaged groups
In studies across the world, researchers investigated what else might make people vulnerable to mental health problems during the pandemic. They found a few key factors that put people at risk.
For one, people with poor health or chronic diseases tend to have higher symptoms of stress, anxiety, depression, and PTSD, several studies found. Of course, this might be because these are also the people with greater health risks from COVID-19.
Your income and education matter, too. The less stable your income and the less educated you are, studies suggest, the more anxiety, depression, and stress you will experience. The pandemic is threatening the economy, affecting everyone’s financial future, but the situation is worse for people who were already struggling. In a very real sense, we’re not all in the same boat.
“It is an inescapable fact that people lower on the socioeconomic ladder are struggling more”
A Pew survey of nearly 5,000 Americans in April found that the lowest-income people were most afraid of getting COVID-19, too. “[While] Americans may be struggling with the emotional challenges of the pandemic, it is an inescapable fact that people lower on the socioeconomic ladder are struggling more,” says psychologist David Sbarra.
6. The effects are compounded by racism
Those unequal effects extend all the way to who lives and who dies.
In fact, Black people are more likely to be infected, less likely to be tested and treated, and less likely to survive if they get COVID-19. According to Andrea King Collier in an article for Greater Good, a history of racism means the Black community is confronting the pandemic with worse health, less access to care, and more distrust of the medical system.
That means they have more reason to be fearful for their own lives, and they are more likely to experience loss. In fact, Pew research suggests that more than a quarter of Black Americans know someone who was hospitalized or died from COVID-19, compared to 1 in 10 white Americans.
These hardships worsened after the police killing of George Floyd, a Black man in Minnesota. His death catalyzed nationwide protests for racial justice—but at the same time, many observers say, it made the pandemic even harder for many Black Americans.
“Black people have been hit on all sides with the threat of loss of life,” says Riana Anderson, assistant professor at the University of Michigan’s School of Public Health. “It is exhausting. Depleting. Depressing. And absolutely an additional stressor.” She argues that family and community support is a strength of the Black community, but physical distancing restrictions have made it more difficult to access that power.
Other people of color are suffering disproportionally under the pandemic, too. Nearly one-fifth of Latino adults were experiencing serious psychological distress in April 2020; the CDC estimates that Latinos make up over half of the U.S. agricultural workforce, a group of essential workers whose jobs put them at greater risk of infection. Discrimination against Asians has risen since the pandemic started in Wuhan, China.
All of these inequities create mental health problems that are even more aggravated by reduced and unequal access to mental health services.
7. Your work situation matters
One of the biggest disruptions to our daily lives today is how the pandemic has affected our work.
Doctors, nurses, and paramedics are taking on the urgent task of caring for COVID-19 patients, while other essential workers are putting themselves at risk to sell food, deliver mail, and pick up trash. Many office jobs have transitioned to remote work, asking employees to isolate at home, with many precariously juggling work and care for children or elders.
Other people have been unable to continue work during the pandemic, waiting for the time when they’ll be called back, while some have been laid off entirely. Unemployment in the U.S. more than quadrupled from February to April, leveling off in July at 10 percent.
A Chinese survey in mid-February examined some of these work situations, though not all. What was clear is that people who are unable to work temporarily—even if they don’t get laid off—have worse mental health. And while working in an office might seem risky, it was the people working from home who were actually more distressed and less satisfied with their lives.
Caring for yourself and others
There’s a lot we don’t have control over in this situation, which is stressful in and of itself. You may have some of the risk factors mentioned above, and there’s nothing you can do about it.
But what can you control? That’s the first question to ask.
For example, research from 28 countries conducted in mid-March found that the more people used social media, the more fearful they were. Frequent social media users in China were more likely to feel both depressed and anxious at the same time. Part of the reason may be because, particularly when the pandemic was ramping up, it was the main topic of discussion online. If being on Facebook doesn’t feel good, consider putting limits on social media time.
Does that mean ignorance is bliss? No. Finding the right sources of information is key. In fact, Chinese people who were highly satisfied with the health information they got about COVID-19 tended to have lower stress, anxiety, depression, and PTSD. Being informed helps reduce uncertainty and anxiety—but overloading ourselves with information can also be unsettling. Online or offline, reading news or imagining worst-case scenarios with family, the people who spent three or more hours a day focusing on COVID-19 were more anxious.
Besides taking breaks from news and social media, practicing basic safety and hygiene could go a long way for your mental health. In Chinese studies in January and February, people who engaged in proper hand washing, wore masks, and avoided sharing utensils tended to experience less depression, anxiety, stress, and PTSD.
Since March, Greater Good has been sharing tips for well-being during COVID-19. For the most part, these are nothing new. In normal life and in a pandemic, we fare better when we try to stay connected in our relationships, cope with stress in healthy ways, and find a sense of agency.
But we can’t self-improve our way out of the pain and difficulty. What we’re going through right now is a trauma, or at least a major stressor on a global scale. This is one of those times when life really is harder by a little bit or a lot, depending on your situation. Feeling bad is part of being human—and right now, that’s something many of us need to face, even as we work to feel better, stay connected, and help others.


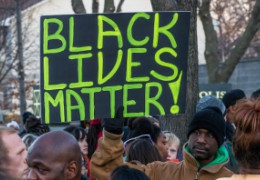






Comments